Consolidation is OVER. Our hospital bag is unpacked and will hopefully stay that way for a long long time. Out of the 63 days of Consolidation, 28 days were spent in the hospital. Turns out, chemotherapy treatment really is tricky! It doesn’t just deceive the leukemia cells from coming back, we were also duped. What is this, some kind of game? Just when we thought we were ahead, prepared for what was coming next – BAM! Chemotherapy scores again! Every time we were discharged, we headed home thinking we had it all figured out. Puke bags ready, pain meds, anti-nausea meds ready, NG tube replacement plan ready. Nope. The intense cocktail of high dose chemotherapy drugs is a raging fire that cannot be contained. We realize that now. It only took us nine weeks but we finally understand that no matter what you THINK may or may not happen, it doesn’t matter. You do your BEST and when that is no longer good enough, you pack your bags and check into Hotel Children’s.
Let’s see, where did we leave off? Oh yes, Consolidation Block #2, The Storm. Well, you can put your tissue boxes away now. But I will warn you to hold from eating while reading this. It may ruin your appetite. I am happy to report that Block #3 while admitted was generally pretty easy. Or maybe it’s just that Block #2 was SO BAD that it made anything after it feel like a breeze. Perspective, right? At least by Block #3 Theo had finally gotten used to the NG tube, making medicine delivery much easier. There were no life threatening allergic reactions and no high dose Methotrexate. The best part? There was no screaming or crying to go home. No, it wasn’t fun, but at least Theo was in good spirits. Uncomfortable yes, but still my sweet boy. It really wasn’t until the last night, day five, that anything out of the ordinary happened. It was our last scheduled day in the hospital. Theo had been feeling good enough to get out of bed and play for at least an hour. We did mutagen experiments with the ninja turtles, completed two puzzles, and made Bobo a birthday card. He was also eating like a champ. Pizza, eggs, pork taco, smoked salmon, rice, apple slices, and ice cream. He drank an outstanding 14 ounces of water, the most he had been able to drink on his own in weeks. Before medicine time he even made a point to tell me how good he felt, how proud he was of himself for eating and drinking so well. His belly was happy. What a great day, what could possibly go wrong? (eye roll) At 9pm the nurse came in to give Theo his last round of scheduled meds, Imatinib included. I have never seen Theo jump out of the bed so fast with his weak legs while attached to the IV pole. The moment Imatinib entered Theo’s stomach he felt the urge to poop and to throw up. Sadly it all happened so fast he never made it to the bathroom. Darn you Imatinib! First big mess, and so it began… helloooo nausea. Recall what I said earlier about being prepared? Right. Well, we thought we were, but this was like no other nausea we had ever seen. Even worse, we were BEHIND it. The key to handling nausea is to be AHEAD of it. The following two weeks was a frustrating game of cat and mouse. Chasing after some problem or ailment and then, just when we thought we had it figured out, we’d start chasing something else that was going wrong. Our heads were constantly spinning, like dogs chasing our own tails. How about you? Is your head spinning yet? I hope not because I’m just getting started!
At discharge on day six, we were giving Theo more anti-nausea meds than usual: Olanzapine at night and Zofran scheduled every eight hours. It seemed to be good enough, up until the dreaded hour of giving Imatinib. He couldn’t keep it down. No matter what we did, no matter what time or how it was delivered. Theo would wake up out of a dead sleep as soon as we started pushing the Imatinib through his NG tube and throw up immediately. We ended up having to give the Imatinib three times on some nights. If a medicine is thrown up within 30 minutes of delivery, it needs to be given again. Those 30 minutes following feeling like eternity. This was a HUGE problem. We could not continue like this, we needed help. We even started to wonder if Theo had developed an allergy to Imatinib… the ONLY drug that can kill the Philadelphia chromosome positive cells.
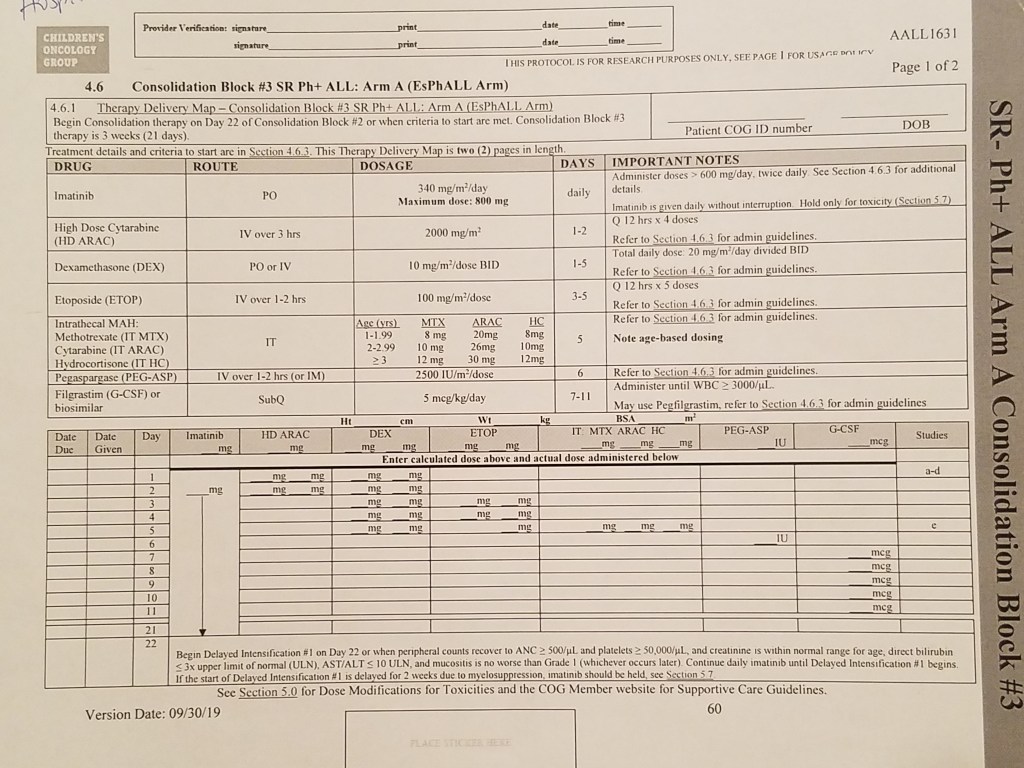
On day seven of Block #3, Theo was scheduled to receive a shot of Nuelasta (chart says Filgastrim). A drug that helps stimulate the bone marrow to start making new cells. That morning Theo could barely speak, he couldn’t stop gagging. Nothing stayed down. After talking to his doctors we were instructed to give him anti-nausea meds every 2-3 hours. WOW, that’s a lot! But it worked. Zofran every eight hours, Benadryl-Reglan and Ativan alternating every six hours. We did this for three days. The only three days Theo held his Imatinib in. Finally! Something that worked. But how long can we go on like this? By the fourth day we decided he was doing better and pulled back on some of the anti-nausea meds, crossing our fingers we weren’t making a big mistake. Phew. We finally made it over the hump of bad nausea. With a transfusion of blood and platelets also completed in that time we were certain he’d be feeling good. We took a deep breath and started to relax a little, ready to enjoy a couple of weeks before the start of the next phase.
What… did you really think that was it?? Ha, that would be too easy. Two days later we were back to anti-nausea meds every 2-3 hours. Theo was back to vomiting and pooping his pants with the Imatinib. Then, the following Monday night the NG tube came out. I tried three times to get it back in but no luck. Not even Theo cheering me on “C’mon Mama, we got this” could make it work. (I am in awe of how well he handles the NG tube placement. Taking deep breaths. So incredibly brave). I think his nose was finally so irritated from the 100 times I had re-inserted the tube. Oh well. With diarrhea, no tube, no Imatinib in, and stomach pain, we had no other option. Off to the the emergency department (ED) we went. Once the Hematology/Oncology clinic is closed, the only way to be admitted is through the ED. I have more on that later, but first… the chase. So one more night admitted and Theo was ready to come home the next day. Or was he? He had kept down all of his meds, even the Imatinib, before we were discharged. We had a solid plan for controlling the nausea. Theo was feeling better with a new NG tube and ready to go home! So WHY did Theo throw up out of the blue at 1am our first night back home and then wake up with a fever? Guess what? That’s right… back to the hospital!!! I bet your head is spinning now!
Here we go again. The chase continues. But what are we chasing now? Nausea? We weren’t so sure anymore. A fever is a sign of an infection. Okay, so it’s more than just nausea. If temperature reaches 100.4 Fahrenheit or 38.0 Celsius, it’s immediate admission. An infection can get very serious very fast. That’s why patients are required to live within one hour of the hospital in case of emergencies. His temperature at home was 101.4 F. When we got to the Hematology/Oncology clinic the nursing assistant got a temperature reading of 98.6 F. Huh? No way, that can’t be right. Hear me out. I am not an expert but I have good reason to not trust temporal thermometers. I know that they are more convenient, especially when a patient is asleep or has been eating food. I was told that a study was done a couple of years ago to see which thermometer method was the best. Temporal thermometers were selected as the superior choice but there has always been some controversy over that decision. Many doctors and nurses that I talked to about this also doubted that decision. Again, I am no expert. But I was starting to notice that the temperature readings I was getting at home (taken orally) were different from the readings at the hospital (taken along the temple). I asked the assistant to retake the temperature under the tongue. 101.4 F. Ahhhh-HA! There it is. So, from then on, I asked for Theo’s temperature to be taken orally, under the tongue.
Theo spent the next three nights in the hospital getting broad spectrum antibiotics, Tylenol, and fluids. Theo was having sudden uncontrollable leaky diarrhea every hour and still throwing up randomly at night. The first night he vomited blood. I was horrified and terrified at the same time. The room looked like a scene from The Exorcist. When Theo was done getting sick he looked around the room, looked at me, then at himself (both covered in the mess) and asked with calm curiosity, “Oh no Mama, how are we going to clean this up?” I would’ve laughed but at that point but I was too busy swearing. What the heck was going on?? The fever was gone. A swab and poop sample were tested for every possible virus that the hospital can test for. They all came back negative. Luis and I were scratching our heads. Drum roll… it was a bug. A BUG?!? Yep, just a bug. Apparently the blood in the vomit was not a “big” deal. Theo’s platelets were low so another platelet transfusion would solve that problem. But what about everything else? Simple answer: neutropenic. *Quick review* A person who is neutropenic has a low level of neutrophils. Neutrophils are a type of white blood cell that fight infection. Neutrophils, red blood cells, other white blood cells, and platelets are made in the bone marrow. Chemotherapy destroys the ability for the bone marrow to make these cells – it wipes away everything bad and good! Intense high dose chemotherpay can wreck so much havoc that neutrophils can be nonexistent for weeks. This is the time infection is most likely to happen. Once the bone marrow recovers, it starts making neutrophils (ANC goes up) and other cells again, then the body can fight bad organisms and rebuild tissues. It takes TIME. Basically, Theo had no inner lining cells to his digestive tract. He was raw inside with no good cells or bacteria to help him out. Just like when he had mucositis, the lining tissues had not been regenerated making it extremely difficult for his body to take in or digest anything. The super thick coating of Imatinib makes it especially hard on the stomach. No wonder it always made him sick. Wow, now it all makes sense.
What a roller coaster ride! We were so relieved to have Theo home and healing with us. For real this time. I promise. Yes, it was challenging and frustrating no doubt. We definitely had a our moments of hair pulling, wall punching anger. But Theo?? I’ve got to hand it to him. He is such a cool cucumber. A true chill master, my sweet little dude. I don’t think I give him enough credit sometimes for how much HE is learning through all of this. How much this whole experience has forced him to deal with pain and discomfort. He is mature beyond his years, a wise old soul. Constantly reminding me to check myself. I can’t tell you how many times he tells me when I am stressed, “it’s okay Mama, just take a deep breath”. We are all learning and growing from this.
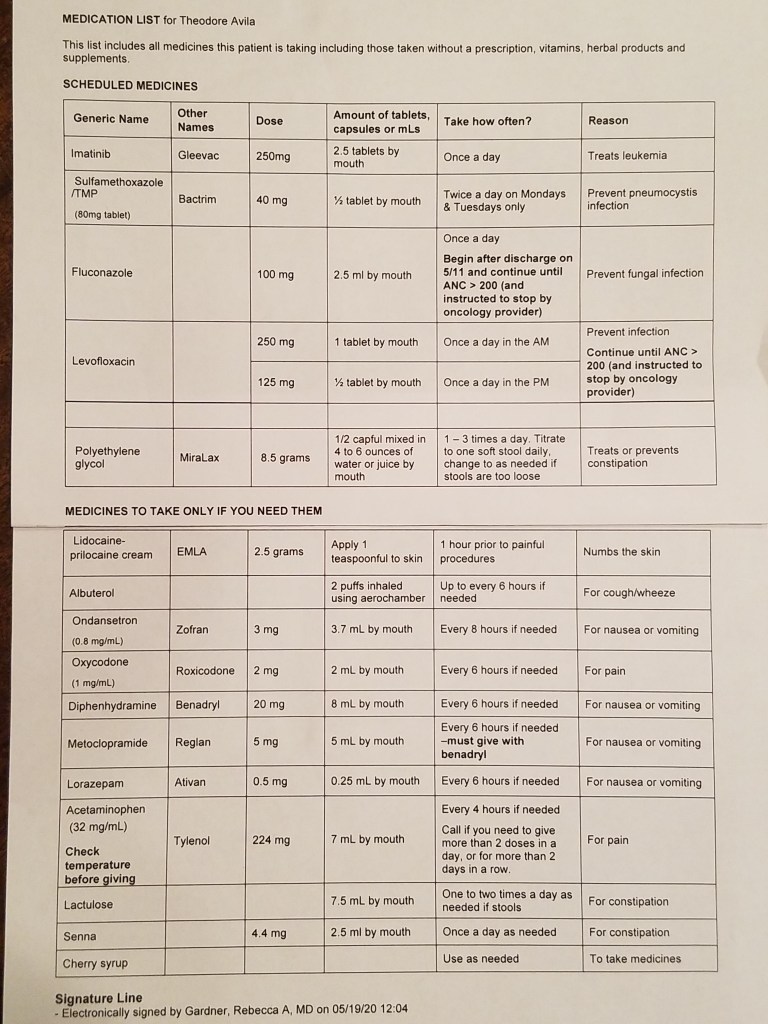
I’d like to talk about an important lesson we learned from this last phase: Ask questions!!! Each time Theo gets admitted to the hospital, we meet another group of doctors, residents, fellows, nurses, etc. Each time we meet someone new we have to repeat the story, the symptoms, the current medicine list (see above)… OVER and OVER. *One night I had to recite Theo’s medicine list three times to three different doctors*. If you have to be admitted through the ED, even worse. The ED is not specialized in treating cancer patients. They are not as familiar with all the meds Theo is taking, his unique treatment, or his specialized needs, like the fact he does NOT like band-aids, but prefers gauze with Kind tape. So when Theo is due for his Zofran or Imatinib and I ask the nurse when he will get it, I get a blank stare in return. One evening during Block #3 while waiting in the ED, I was told Theo couldn’t eat past 12am (NPO) because he had a “possible procedure” the next day. Huh?? I was persistent in telling the nurse and doctors that he had NO procedure scheduled until July 7th – one week out. The procedure being a lumbar puncture of chemotherapy into his spinal fluid, aka, the start of his next phase of treatment. Why was this suddenly on the schedule? The resident on staff in the ED noticed the note in Theo’s chart that the procedure was set for one week out so he/she decided that perhaps it should just be done one week earlier, since we were already there… for our convenience. REALLY?!?! You think giving my son, who is checking into the hospital for nausea and diarrhea, who’s ANC is little to nothing, should have MORE chemotherapy one week early?? That is the opposite of convenient. That is thoughtless. He is in the hospital to HEAL!! Ugh.. that had me fuming out of the ears. There were other times as well, when Luis or I had to intervene. What can I say. You need to be on top of it. You need to know what’s going on. You need to KNOW the meds. You need to ASK QUESTIONS!!! At Children’s Hospital we are surrounded by so many brilliant minds, countless doctors and nurses who care deeply and want to help. Everyone is doing their best and we are so grateful. It’s just that we are so used to the the unique specialized care and attention we get from the Hematology/Oncology clinic. They are OUR PEOPLE. Theo’s doctors know him SO well. They know his journey inside and out, his strengths, his weaknesses, his struggles. They have a pharmacist who specializes in the medicines used to treat cancer. They even know the names of all his stuffies, for goodness sake! We are so spoiled by them all. Bottom line: everyone at Children’s Hospital is there to help, to care for Theo, and they all want what’s best for him. Just remember… ASK QUESTIONS!!!
I had a nightmare. I was drowning. Swallowed into a blur of blue and black. My body felt heavy, like something was pulling me down, further, deeper, darker. The water was thick like oil. I could not see light. I could not see anything. I don’t know how I got there or when it all started. But I never stopped fighting, never stopped trying to escape the weight of the water holding me under. Suddenly there was air. I took the deepest most luxurious breath in. I filled my lungs up with happiness and my body was still. Is that the end? Am I safe? For now, yes. Today I have both feet firmly planted on the ground. Today I breathe with awareness and intention. Today I embrace the pure essence and joy of Theo. How is Theo? Today he is laughing, playing, and even eating. Tomorrow… we will see. Every day he is my super hero.

“No matter what you step in, keep walking along and singing your song… because it’s all good.” – Pete the Cat, I Love My White Shoes, by Eric Litwin
Sending you all strength, healing, happiness, love & big safe, virtual hugs!!! ❤️❤️❤️
LikeLike